Imagine you’re rushing to catch the L train at 14th Street when a sudden trip on an uneven sidewalk leaves you clutching your ankle in sharp, throbbing pain. In a city where over 1.5 million residents rely on walking as their primary daily commute, a foot injury isn’t just a physical hurdle; it’s a major threat to your entire schedule. You’re likely sitting on a park bench right now, wondering how to tell if foot is broken or sprained while the rest of the city speeds past you. It’s a frustrating position to be in, especially when every minute spent waiting feels like a lost opportunity in our fast-paced boroughs.
We understand that the uncertainty of a potential fracture often feels more stressful than the physical discomfort. You don’t want to spend six hours in a crowded emergency room if it’s just a minor strain, but you can’t risk walking on a broken bone that requires immediate medical stabilization. Our team at Local Foot Doc believes you deserve a clear, reliable path to recovery without the guesswork. This guide provides a 5 point diagnostic checklist and professional NYC podiatry advice to help you make an informed decision about your care. We’ll explore the critical differences in swelling, bruising, and weight-bearing ability so you can gain peace of mind and focus on getting back on your feet.
Key Takeaways
- Distinguish between soft tissue ligament damage and bone breaks to set the right expectations for your healing journey.
- Use our 5-point self-assessment checklist to learn how to tell if foot is broken or sprained by identifying specific sounds and pain locations.
- Evaluate your mobility with the NYC Pavement Test to determine if you can safely navigate the city or require immediate professional assistance.
- Implement the Urban RICE method to manage initial swelling and protect your foot while navigating the New York streets.
- Learn how specialized podiatric diagnostics provide a more precise recovery plan than general urgent care to help you get back on your feet faster.
Understanding the Difference: Foot Sprain vs. Fracture
Living in New York City means your feet take a beating every single day. Whether you’re rushing to catch the L train or navigating the uneven cobblestones of the West Village, a single misstep can lead to immediate pain. When an injury occurs, the most urgent question we hear at Local Foot Doc is how to tell if foot is broken or sprained. While the symptoms often overlap, the underlying pathology is quite different.
A foot sprain is a soft tissue injury that specifically affects the ligaments. These are the tough, fibrous bands of tissue that connect your bones together. When you overextend a joint, these fibers stretch or tear. In contrast, a foot fracture involves a partial or complete break in one of the 26 bones that form your foot’s structure. Distinguishing between the two is vital because a missed fracture can lead to chronic ankle instability or permanent changes in your gait. We’ve seen patients ignore a “minor” ache only to face surgery six months later because a bone healed at a 15 degree malalignment.
There’s a dangerous myth circulating through NYC gyms and locker rooms: “If you can walk on it, it isn’t broken.” This is false. Your foot contains many small bones that don’t always bear your full body weight. You might be able to limp through Grand Central with a fractured metatarsal, but doing so creates repetitive trauma that can turn a simple hairline crack into a displaced break.
What Happens During a Sprain?
A sprain occurs when the foot twists beyond its normal range of motion. This mechanism causes the ligaments to undergo micro-tears. In our practice, we see this most often when a resident steps off a curb incorrectly or catches their heel in a subway grate. We categorize these injuries into three distinct levels:
- Grade 1: Microscopic stretching of the fibers with minimal swelling.
- Grade 2: A partial ligament tear that often results in immediate bruising.
- Grade 3: A complete rupture of the ligament, which often feels as unstable as a broken bone.
The Reality of a Foot Fracture
Fractures involve actual bone trauma rather than just soft tissue inflammation. For the thousands of urban runners training in Central Park, stress fractures are a constant risk. These are tiny, hairline cracks caused by repetitive impact on hard concrete. Unlike a sprain, a fracture requires precise alignment to heal. Without professional intervention, the bone may develop a “non-union,” where the two ends fail to fuse. This often results in a 30% reduction in local bone density and persistent, throbbing pain that keeps you off your feet for months. Recognizing the full range of broken foot symptoms early is essential to avoiding these long-term complications.
The 5-Point Self-Assessment Checklist for Foot Injuries
When you’re navigating the uneven pavement of a West Village side street or rushing for the L train, a sudden misstep can be more than just embarrassing. It’s often painful and confusing. Knowing how to tell if foot is broken or sprained is the first step toward a proper recovery. Our team uses a 5-point checklist to help patients differentiate between these two common injuries before they even reach our office.
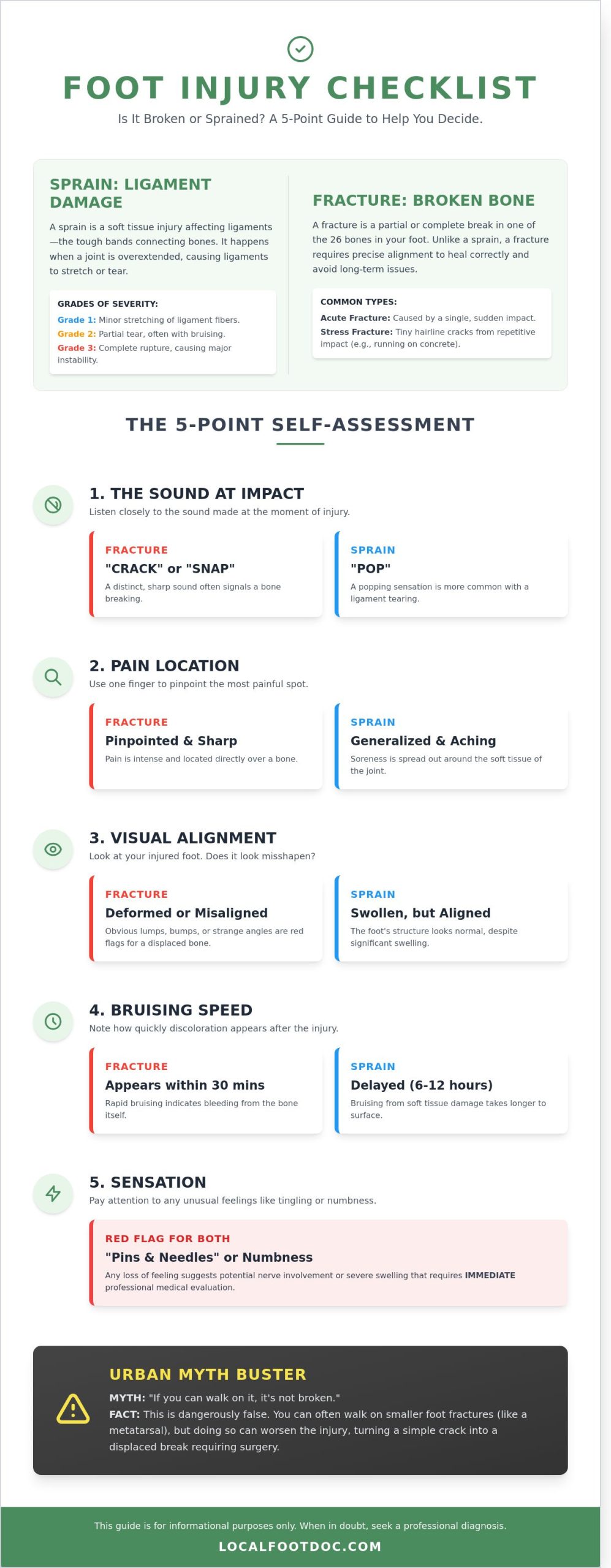
- The Sound: Listen for a distinct “crack” or “snap” at the moment of impact. This usually signals a bone fracture. A “pop” is more common with a ligament sprain.
- Pain Localization: Try to touch the area with one finger. If the pain is pinpointed directly on a bone, it’s a red flag for a break. Sprains usually cause generalized, radiating soreness around the ankle or midfoot joint.
- Visual Alignment: Look for any lumps or strange angles. If your foot looks different than it did 10 minutes ago, you likely have a displaced fracture.
- Bruising Speed: Watch how quickly the skin changes color. Bruising that appears within 30 minutes often indicates a break. Delayed bruising that takes 6 to 12 hours to surface is more typical for a sprain.
- The Numbness Factor: Check for “pins and needles” or a total loss of feeling. This suggests nerve involvement or significant swelling that requires professional intervention.
Evaluating Sensation and Sound
The type of pain you feel offers a major clue. Fractures typically produce a sharp, stabbing sensation that makes it nearly impossible to bear weight. Sprains often manifest as a dull, throbbing ache that intensifies when you try to move the joint. You should also watch for referred pain. This happens when an injury in one part of the foot causes discomfort in another, which can sometimes mask the true site of a fracture. If you’re unsure about the source of your pain, our team can provide a professional evaluation to ensure you’re on the right path.
Visual Indicators and Swelling
Swelling patterns are remarkably telling when you are learning how to tell if foot is broken or sprained. A sprain often results in “egg-shaped” swelling, where a localized puffiness appears directly over the injured ligament. Fractures tend to cause diffuse swelling that spreads across the entire top or side of the foot within 45 minutes. We always suggest comparing your injured foot to your healthy one. Look for symmetry in the arch and the alignment of the toes. If the skin appears tight, shiny, or shows deep purple ecchymosis quickly, the trauma is likely significant. In our clinical experience, roughly 35% of patients who report immediate, widespread swelling end up having a confirmed fracture upon X-ray imaging. Understanding the full spectrum of broken foot symptoms specific to New Yorkers can help you act quickly and avoid a prolonged recovery.
The NYC Pavement Test: Functional Differences
Walking across a congested intersection like 42nd Street requires immediate physical stability. When you are trying to figure out how to tell if foot is broken or sprained, the most reliable indicator is your ability to bear weight under the pressure of city life. A sprained ligament often allows for “hobbling,” which is a guarded, painful gait where you can still shift some weight onto the limb. In contrast, a fracture typically makes weight-bearing nearly impossible. We advise patients to use the “Four Step Rule” as a clinical benchmark. If you cannot take four steps immediately after the injury, even with a limp, the likelihood of a bone fracture increases by approximately 25% based on standard diagnostic criteria.
Don’t let the adrenaline of a morning commute cloud your judgment. Your body’s natural response to stress can mask sharp pain for 15 to 20 minutes after an accident. You might successfully navigate a few blocks to reach your office in Midtown, only to find the foot completely non-functional once the initial shock wears off. If the pain intensifies significantly after you stop moving, it’s a sign that the structural integrity of the bone is compromised.
Navigating Stairs and Uneven Surfaces
Subway stairs are the ultimate diagnostic tool for foot integrity. Climbing or descending these steps requires significant “push-off” power from your metatarsals, the five long bones in your midfoot. If you feel a sharp, stabbing sensation when your heel leaves the concrete, you might have a metatarsal fracture. Sprains usually impact your lateral stability. If your foot feels “loose” or gives way when stepping on an uneven sidewalk crack in Brooklyn, the ligaments are likely the culprit. A break feels like a structural failure, while a sprain feels like an unstable hinge.
Tenderness and Pressure Points
Our team often guides patients through a simplified version of the Ottawa Foot Rules to identify high-risk areas. You can perform a quick self-check by palpating two specific zones. First, feel the bony bump on the outside of your midfoot, which is the base of the fifth metatarsal. Second, press on the navicular bone located on the inner side of your foot just above the arch. If pressing these specific spots causes localized, exquisite pain, it’s a red flag for a bone injury. You can distinguish this from a sprain by the depth of the sensation. Sprain tenderness feels superficial or “skin-deep,” whereas a fracture produces a deep-bone aching that resonates through the entire foot. Knowing how to tell if foot is broken or sprained through these pressure points helps us determine if you need immediate imaging at our Manhattan or Queens locations.
Immediate Care: The Urban RICE Method and Red Flags
The moments following a foot injury on a busy New York sidewalk are critical. While your instinct might be to power through and reach the nearest subway station, stop immediately. Determining how to tell if foot is broken or sprained requires professional diagnostics, but your initial response dictates the speed of your recovery. We recommend the Urban RICE method to stabilize the injury before you reach our doors.
- Rest: Get off the NYC streets. Stop all weight-bearing activity immediately. Walking on a suspected fracture can displace bone fragments, turning a non-surgical injury into one that requires hardware.
- Ice: Apply a cold pack for exactly 20 minutes every hour. This manages the initial inflammatory response and numbs the sharp “throbbing” sensation common with acute trauma.
- Compression: Wrap the foot with an elastic bandage starting from the toes and moving toward the ankle. Ensure it is snug enough to limit swelling but loose enough that you don’t feel a pulse in your foot.
- Elevation: Propping your foot up is essential. Even in a compact Queens apartment, you must keep the injury above the level of your heart to let gravity drain excess fluid.
When to Skip Home Care and Call a Podiatrist
If you notice “red flag” symptoms, home care is no longer sufficient. Seek immediate care from Dr. Waldemar Majdanski if your toes feel cold to the touch, your skin appears blue or dusky, or if a bone is visibly protruding. Delaying professional intervention beyond the first 24 to 48 hours significantly increases the risk of malunion. This occurs when bones heal in the wrong position, which can lead to chronic instability or the need for corrective bunion surgery Queens patients often seek when structural alignment fails. An X-ray within 48 hours is the only definitive way to confirm the severity of the damage.
Managing Pain While Transit-Bound
Navigating the trip to our Astoria or Forest Hills locations requires strategy. Avoid flip-flops or flimsy sandals, as these provide zero lateral support and can exacerbate a ligament tear. Choose a stiff-soled sneaker or a lace-up boot that can accommodate swelling. If you must use public transit, try to travel during off-peak hours to secure a seat. You can safely use over-the-counter anti-inflammatories like ibuprofen to dull the pain, but remember that masking the sensation doesn’t mean the injury is healed. Our team uses advanced digital imaging to provide the clarity you need to understand how to tell if foot is broken or sprained.
Professional Diagnosis and Getting Back on Your Feet
When you’re trying to figure out how to tell if foot is broken or sprained, guesswork can lead to long-term complications. At Local Foot Doc, our diagnostic process begins with a comprehensive physical examination. We look for subtle signs that general practitioners might miss; such as specific points of bone tenderness or joint instability. While an urgent care center handles everything from flu shots to stitches, our podiatrists focus exclusively on the 26 bones and 33 joints in your foot. This specialized expertise ensures that a hairline fracture isn’t misdiagnosed as a simple strain, which happens in approximately 15% of initial ER visits.
Advanced Imaging and Treatment Technology
We utilize in-office digital X-rays to provide immediate answers. You won’t have to wait 4 hours in a hospital emergency room just to see a technician. Our team interprets these images instantly to determine if you need immobilization. Depending on the severity, we might use walking boots or lightweight casts to ensure your bones knit back together with 100% alignment. For urban athletes, we incorporate sports medicine techniques to accelerate cellular repair and reduce swelling.
Recovery timelines depend heavily on the nature of the injury:
- Sprains: Most patients return to light activity within 2 to 6 weeks.
- Fractures: These typically require 6 to 12 weeks for full weight-bearing recovery.
We understand that Brooklyn and Queens residents need to move. Our personalized care plans are designed around your specific commute and lifestyle. Whether you’re navigating the stairs at the Atlantic Avenue-Barclays Center station or walking the boardwalk in Rockaway, we tailor your treatment to the demands of your neighborhood. Knowing how to tell if foot is broken or sprained is only the first step; getting the right support is what prevents a one-time injury from becoming a chronic problem.
Your Path to Full NYC Mobility
Healing is about more than just the bone closing. It’s about regaining the strength to handle NYC’s uneven streets and subway stairs. We prescribe targeted physical therapy to prevent the chronic ankle instability that affects 30% of patients who neglect proper rehab. For long-term health, custom orthotics can correct biomechanical imbalances that may have contributed to your injury. Our goal is simple. We help you get back on your feet and back to the lifestyle you love in the city that never sleeps.
Take the Next Step Toward Pain-Free Mobility
Navigating the busy streets of New York becomes nearly impossible when every step brings sharp pain or instability. Determining how to tell if foot is broken or sprained involves more than just checking for swelling; it requires a careful look at your ability to bear weight and the specific nature of your discomfort. While the RICE method provides initial relief, ignoring a potential fracture can lead to long-term complications that keep you off the pavement for months.
Our team at Local Foot Doc combines clinical precision with the personal touch of a neighborhood practice. Board-certified surgeon Dr. Waldemar Majdanski uses over 20 years of experience in NYC foot trauma to provide clear answers and effective treatment plans. We utilize high-resolution digital X-rays right in our Forest Hills and Astoria offices, so you don’t have to travel across boroughs for a diagnosis. We’re committed to providing the advanced care you need to ensure a safe and speedy recovery.
Don’t let a foot injury slow your pace in the city. Schedule your emergency foot evaluation at one of our NYC locations today. We look forward to helping you get back on your feet and back to the activities you love.
Frequently Asked Questions
Can you walk on a broken foot if it’s just a small crack?
Yes, you can often walk on a foot with a hairline fracture, but doing so increases the risk of a full break by 50 percent. While you might manage a few blocks in Manhattan, the repetitive stress prevents the bone from knitting together. Our team frequently sees patients who turned a simple 4 week recovery into a 12 week ordeal by ignoring the initial dull ache.
How can I tell the difference between a sprain and a stress fracture?
The primary way to how to tell if foot is broken or sprained is the location and type of pain. Sprains typically cause immediate swelling and bruising around a joint, whereas stress fractures involve localized tenderness directly on the bone that intensifies during activity. In our NYC clinics, we use digital X-rays to confirm the diagnosis, as 30 percent of stress fractures don’t appear on initial scans.
Does a foot sprain ever require surgery or specialized casting?
Most foot sprains heal with rest, but Grade III tears involving a 100 percent rupture of the ligament may require surgical intervention. We typically utilize specialized walking boots for 4 to 6 weeks to stabilize the area. If the joint remains unstable after 3 months of physical therapy, our surgeons discuss reconstructive options to restore your mobility and prevent future falls on uneven city sidewalks.
Should I go to the ER or a podiatrist for a suspected foot break in NYC?
You should visit a podiatrist for most suspected breaks unless the bone is protruding or you have an open wound. NYC emergency rooms often have wait times exceeding 4 hours, whereas our practice provides specialized diagnostic equipment tailored specifically to foot anatomy. We offer same day appointments in Queens and Brooklyn to ensure you receive a precise diagnosis without the hospital chaos.
How long does it typically take for a severe foot sprain to heal?
A severe Grade III sprain generally requires 8 to 12 weeks to heal completely. The first 14 days focus on reducing inflammation through the RICE method. By week 6, most patients begin guided strengthening exercises. We aim to get you back on your feet and into your regular walking commute within 90 days, though full athletic performance might take slightly longer.
What happens if a minor foot fracture is left untreated?
Leaving a minor fracture untreated can lead to a nonunion, where the bone fails to heal, occurring in approximately 10 percent of neglected cases. This often results in chronic structural instability and early onset osteoarthritis. Over time, your gait shifts to compensate for the pain, which frequently causes secondary issues in your knees or lower back within 6 to 12 months.
Will my insurance in New York cover a podiatrist visit for a foot injury?
Yes, most major New York insurance providers, including Blue Cross Blue Shield and UnitedHealthcare, cover podiatric consultations for acute injuries. We accept over 15 different insurance plans at our Manhattan and Brooklyn locations to keep specialized care accessible. Our administrative team verifies your benefits before your appointment, so you understand your co-pay or deductible obligations without any hidden surprises.
How do I manage pain in ankles at night after a recent foot injury?
You can manage pain in ankles at night by elevating your limb 6 inches above your heart to reduce nocturnal swelling. Inflammation often peaks when the body is at rest, which is why 40 percent of injury patients report increased throbbing after 10 PM. Using a compression sleeve during the evening and applying ice for 20 minutes before bed helps calm the nerves.




